Privacy Policy for Users of GayToday.com
Badpuppy Enterprises, Inc.
5505 N. Atlantic Ave. #204
Cocoa Beach, FL 32926
USA
Phone: 321.631.9500
Data Protection Officer: Jeff Goodrich, support@badpuppy.com
Last Updated: May 20, 2018
GDPR Notice
A strong relationship with our users is essential. A critical part of these relationships is establishing trust and confidence, which is why the privacy and security of your data has always been our priority for over 23 years. Over the last few months we have worked to get all of our web properties secured by HTTPS. We have secured not just the Contact, Login and Registration forms; but, your entire surfing experience is safe.
With the General Data Protection Regulation (GDPR) set to take effect on May 25, 2018 we are in the process of deploying updates allowing us to comply with new regulations and ensure people can continue using BEI (Badpuppy Enterprises, Inc.) properties with confidence. Although GDPR applies only to data collected from persons located in the European Union (EU), our goal is to continuously implement network-wide improvements and new functionalities for all BEI users.
If you notice an area of our site where you feel we can do a little better, please don't hesitate to contact us.
Overview
Your privacy is very important to us. We do not sell or rent your personal information to third parties for any reason without your explicit consent.
Please read this privacy policy to learn about the ways in which we use and protect your personal information. The privacy practices of this statement
apply to our services available under the domain and subdomains of www.Badpuppy.com (the "Site"). By visiting this website you agree to be bound by the
terms and conditions of this Privacy Policy. If you do not agree, do not use or access our Site.
-
Children (persons under the age of 18, and in some cases 21, where applicable) are not eligible to use our Site and we require that children do not
submit any personal information to us.
-
Information We May Collect and How We Collect It:
Our primary goal in collecting personal information is to provide you with a smooth, efficient, and customized experience. This allows us to provide services and features that most likely meet your needs, and to customize our service to make your experience easier. We only collect personal information about you that we consider necessary to achieve that purpose. We do not now, nor have we ever, used any form of tracking for purposes of delivering advertising to our users.
We may collect several types of information from and about users of our Site, including information:
- by which you may be personally identified, such as first and last name, mailing address, email address, billing information, IP or “Internet Protocol” addresses, demographics, passwords or other online contact information, telephone number, any other information the Site collects that is defined as personal or personally identifiable information under applicable law or other identifier by which you may be contacted online or offline (“personal information”);
- that is about you but individually does not identify you; or
- about your internet connection, the equipment you use to access our Site, usage details (such as the web pages you visit, links on which you click, and the searches you conduct on our Site), your browser type and language, access times, and the content of any undeleted cookies that your browser previously accepted from us.
Information may be collected:
- directly from you when you provide it to us,
- if other users or third parties send us correspondence about your activities or postings on the Site,
- automatically, as you navigate through the site. Information collected automatically may include usage details, IP addresses and information collected through cookies, web beacons or other tracking technologies, or
- from third parties, for example, other websites controlled by us or our affiliates, our business partners or other third parties.
-
Our Use of Your Information:
We use information in the file we maintain about you, and other information we obtain from your current and past activities on the website, to resolve disputes, and troubleshoot problems. At times, we may look across multiple users to identify problems or resolve disputes, and in particular we may examine your information to identify users using multiple User IDs or aliases. In general, we use information that we collect about you or that you provide to us, including any personal information:
- to enforce our Terms of Service;
- to properly display our Site and its content to you;
- to provide you with information, products or services that you request from us;
- to notify you about changes to our Site or any products or services we offer or provide though it;
- to manage your account and provide you with customer support;
- to perform research and analysis about your use of, or interest in, our products, services, or content, or products, services or content offered by others;
- to provide you with notices about your account or subscription, including expiration and renewal notices;
- to track usage throughout various components of the Site (e.g., tracking where traffic comes from, how traffic flows within the Site, etc.);
- to communicate with you about products or services that may be of interest to you either from us, our affiliates or other third parties;
- to verify your eligibility and deliver prizes in connection with contests and sweepstakes;
- to manage our business;
- to monitor aggregate metrics such as total number of visitors, pages viewed, demographic patterns, etc.;
- to allow you to participate in interactive features on our Site;
- to determine whether users of the Site are unique, or whether the same user is using the Site on multiple occasions;
- to develop and display content and advertising tailored to your interests on our Site and other sites;
- in any other way we may describe when you provide the information;
- diagnose or fix technology problems; or
- for any other purpose with your consent.
-
Our Disclosure of Your Information:
Due to the existing regulatory environment, we cannot ensure that all of your communications and other personally identifiable information will never
be disclosed in ways not otherwise described in this Privacy Policy. By way of example (without limiting the foregoing), we may be forced to disclose
information to the government or third parties under certain circumstances, third parties may unlawfully intercept or access transmissions or private
communications, or users may abuse or misuse your information that they collect from our Site. Therefore, although we use industry standard practices
to protect your privacy, we do not promise, and you should not expect, that your personally identifiable information or private communications will
always remain private.
We do not share your personal information with others except as indicated below or when we inform you and give you an opportunity to opt out of having your personal information shared:
- To our authorized service providers that perform certain services on our behalf. These services may include fulfilling orders, processing credit card payments, risk and fraud detection and mitigation, providing customer service and marketing assistance, performing business and sales analysis, supporting our Site functionality, and supporting contests, sweepstakes, surveys and other features offered through our Site. These service providers may have access to personal information needed to perform their functions but are not permitted to share or use such information for any other purposes.
- To a buyer or other successor in the event of a merger, divestiture, restructuring, reorganization, dissolution or other sale or transfer of some or all of our assets, whether as a going concern or as part of bankruptcy, liquidation or similar proceeding, in which personal information held by us about our Site users is among the assets transferred.
- To third parties to market their products or services to you if you have consented to these disclosures.
- To fulfill the purpose for which you provide it.
- For any other purpose disclosed by us when you provide the information.
- With your consent.
-
Control of Your Password:
You are responsible for all actions taken with your User ID and password. Therefore, we do not recommend that you disclose your Badpuppy.com password to
any third parties. If you choose to share your User ID and password or your information with third parties, you are still responsible for all actions
taken with your User ID and password. If you lose control of your password, you may lose substantial control over your personally identifiable
information. Therefore, if your password has been compromised for any reason, you should immediately change your password,
-
Reviewing and Changing Your Personally Identifiable Information:
Following registration, you can review and change the information you submitted during registration by contacting support@badpuppy.com. Once posted, you cannot change or remove any public postings made in the feedback areas.
- Deactivation & Deletion of Information:
Upon your request, we will deactivate your account and contact information from our active databases. To make this request, email support@Badpuppy.com.
Such information will be deactivated as soon as reasonably possible in accordance with our deactivation policy and applicable law.
-
How Long Do We Store Your Data:
Non-public data related to your account and any financial transactions are kept indefinitely. User generated data is maintained until removal is requested by the user.
-
Our use of Cookies and other Tracking Technologies:
Some content or applications on the Site require the use of Cookies for purposes of delivering and formatting content on your screen. Please see our Cookie Policy for further information.
-
Third-Party use of Cookies and other Tracking Technologies:
Some content or applications, including advertisements, on the Site are served by third parties, including advertisers, ad networks and servers, content providers and application providers. These third parties may use cookies alone or in conjunction with web beacons or other tracking technologies to collect information about you when you use our Site. The information they collect may be associated with your personal information or they may collect information, including personal information, about your online activities over time and across different websites and other online services. They may use this information to provide you with interest-based (behavioral) advertising or other targeted content.
We do not control these third parties’ tracking technologies or how they may be used. If you have any questions about an advertisement or other targeted content, you should contact the responsible provider directly.
-
Security - How We Protect Your Data:
Badpuppy.com uses industry standard practices to safeguard the confidentiality of your personal identifiable information. Badpuppy.com treats data as
an asset that must be safeguarded against loss and unauthorized access. We employ several different security techniques to protect such data from
unauthorized access by users inside and outside the company. However, "perfect security" does not exist on the Internet.
We take appropriate security measures (including physical, electronic and procedural measures) to help safeguard your personal information from unauthorized access and disclosure. For example, only authorized employees are permitted to access personal information, and they may do so only for permitted business functions. In addition, we use encryption in the transmission of your sensitive personal information between your system and ours, and we use firewalls to help prevent unauthorized persons from gaining access to your personal information.
The safety and security of your information also depends on you. Where we have given you (or where you have chosen) a password for access to certain parts of our Site, you are responsible for keeping this password confidential. We ask you not to share your password with anyone. We urge you to be careful about giving out information in public areas of the Site like message boards. The information you share in public areas may be viewed by any user of the Site.
-
Data Breach:
In the event of a Data Breach all parties will be notified within 72 hours of discovery, where feasible. Notification may be sent via email, text message, physical mail or any other means of expeditious contact.
-
User Contributions:
We may provide areas on the website where you can post information about yourself and others and communicate with others, upload content (e.g., text, pictures, videos, audio files, etc.), and post comments or reviews of content found on the website. Such postings are governed by our Terms of Services located at https://GayToday.com/index.php/terms-of-service. If you use a forum, blog, bulletin board, channel, chat room, user commenting features, or other interactive sharing or social features that may be offered through our Site, you should be aware that any personal information you submit, display, or publish there is considered publicly available and can be read, collected, used, and disclosed by other users of those features, by us, and other third parties without restriction, except to the extent limited access features are available, if any. In addition, such postings may appear on other websites or when searches are executed on the subject of your posting. If you post your email address, you may receive unsolicited messages. We cannot control who reads your posting or what other users may do with the information you voluntarily post, so we encourage you to exercise discretion and caution with respect to your personal information. Once you have posted information, you may not be able to edit or delete such information. To request removal of your personal information from our blog, sharing service or community forum, for example, send us an e-mail at support@badpuppy.com. In some cases, we may not be able to remove your personal information, in which case we will let you know if we are unable to do so and why.
-
Notice:
We may change this Privacy Policy from time to time based on your comments and our need to accurately reflect our data collection and disclosure
practices. All changes to this policy are effective after we post the changes on our Site.
|
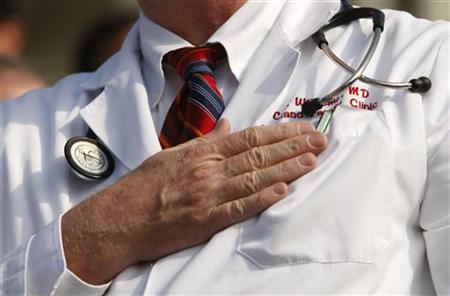 Government health benefits for some 9 million of the sickest and poorest U.S. citizens will come under scrutiny from the congressional “super committee” seeking to cut the nation’s debt.These are Americans who qualify for both the Medicare and Medicaid programs for the elderly and the poor, based on their disability, age and low income.
Government health benefits for some 9 million of the sickest and poorest U.S. citizens will come under scrutiny from the congressional “super committee” seeking to cut the nation’s debt.These are Americans who qualify for both the Medicare and Medicaid programs for the elderly and the poor, based on their disability, age and low income.